Clarity RCM at a Glance
The largest independent dermatology RCM company in the country. Built by derm, for derm.
Results That Speak for Themselves
| Metric | Clarity RCM | Industry Average |
|---|---|---|
| Net Collection Rate | 98% | ~90% |
| Days in A/R | 23-day average | ~45 days |
| First-Pass Clean Claim Rate | 98%+ | ~85% |
| Average Revenue Uplift | 118% | N/A |
| Charge Submission Turnaround | 24-48 hours | 3-4 days |
| Client Retention | 98% | N/A |
Full Revenue Cycle Management
Everything from charge entry to collections, plus strategic advisory.
Charge Entry & Claims
Same-day submission, 24-48 hour turnaround. Custom derm-specific scrub rules and denial-trend algorithms.
Denial Management
Full audit response for TPE, RAC, UPIC, and ADR. Appeals management with derm-specific expertise.
Payment Posting
Insurance and patient payments. Integrated with ClarityPay for patient billing and collections.
Credentialing
End-to-end credentialing management. Payer enrollment, ERA/EFT setup via TriZetto.
Financial Reporting
CEO-level dashboards and analytics. Benchmark library with NCR, DSO, FPRR, and 90+ A/R tracking.
Patient Services
Dedicated patient billing support. EOB explanations, payment plans, and phone/text support at 502-480-1940.
Three Pillars of Differentiation
Deep Derm Expertise
- Certified dermatology coders
- Custom derm-specific scrub rules
- Benchmark library across 200+ practices
- 100% dermatology focus
High-Touch Control
- Clients feel empowered, not outsourced
- Live dashboards and transparent reporting
- Dedicated senior account manager
- Named pod assigned to each practice
Practice Partnership
- Transfer best practices from top groups
- Advisory playbooks (no-shows, payer mix)
- M&A and growth strategy support
- No nickel-and-diming for strategic advice
Positioning & Messaging
The strategic messaging framework behind everything we say. Know this cold.
Anchors
Most dermatology practices lose significant revenue because billing is handled by under-resourced in-house teams or by other RCM vendors that lack true dermatology scale and leadership-level partnership.
Three Differentiation Pillars
Pillar 1: We turn our dermatology expertise and scale into your advantage
- Unmatched volume to recognize patterns across procedures, payers, and practice models before they become denials
- Derm-specific KPI and benchmarks so owners can run the practice like a CEO
- Same-day submission, fix issues at root, continuously tune scrub rules
Pillar 2: We give you a high-touch expert team that keeps you in control
- Seasoned AM and named pod that operate as your team and own outcomes
- Frequent, proactive reviews, alerts, and transparent reporting
- Tailored workflows to your systems
Pillar 3: We help the whole practice thrive, not just billing and coding
- Transfer best practices from top derm groups into operations, finance, and growth plans
- Provider compensation models and patient-pay policies
- End-to-end credentialing, payer strategy, audit-readiness
Clarity is the dermatology revenue-cycle partner for practices that want to thrive. We pair unmatched specialty scale and analytics with a seasoned, high-touch team and a practice-management partnership that goes far beyond billing. The result is clean claims, denials fixed at the root, CEO-level visibility, and a growth engine you control.
Messaging Hierarchy
ClarityOS: What’s Coming
Everything your practice needs to stay ahead, in one place.
Your practice’s money, in real time.
ClarityOS gives dermatology practice owners a single live view of collections, A/R, payer performance, and patient payments. No more waiting on reports.
- Live dashboards replace PDFs and spreadsheets. Collections, denials, payer performance – updated as it happens.
- Financial data, patient payments, benchmarks, and team communication. No more toggling between email, portals, and phone calls.
- Built by the team that runs revenue cycle for more dermatology practices than anyone. Eight years of specialty billing knowledge, now in your hands.
Early access waitlist is live:
os.clarityrcm.comInc. 5000 Three Years Running
#1094 (2023) · #855 (2024) · #1298 (2025) among America’s fastest-growing private companies. 100% growth powered by word of mouth.
The Elevator Pitch
Ashwin’s framing. Works in any conversation.
Key Phrases
From Ashwin. Keep these ready.
Two Audiences, Two Approaches
Reassuring & Grounded
Confident & Forward-Looking
Existing Client Conversations
“Can you tell me more about ClarityOS?”
“I’m talking to SubQ Docs next week”
Don’t call SubQ Docs a partner or position us as complementary. We’re open to working with any EHR or documentation tool, but we’re not cheerleading for them.
Our View on Clinical
When EHR or clinical documentation questions come up. Keep this to five sentences max.
“There are a lot of companies focused on scribing and clinical documentation. There are a lot more focused on getting big health systems paid. We’re focused on something specific: getting small, independent derm practices paid for their services and helping them run their business better. That’s a different problem, and it’s the one we’ve spent eight years solving.”
“Our goal is to be a full practice platform. We’re building from the financial layer up – revenue cycle, dashboards, patient payments – and expanding from there.”
“We think the financial side is where independent practices need the most help right now. That’s our starting point.”
AAD Booth – March 27–31, Denver
Where the bulk of your conversations will be with non-clients. Be more audacious here.
Booth 1515
10x20 peninsula, next to CareCredit, across from Galderma
Espresso Bar
Fri + Sat – barista, Clarity-branded sleeves
60″ TV
Sizzle reel looping (26–35s, no audio)
Mac Minis
Clickable ClarityOS prototype for demos
Sizzle Reel vs. Prototype
Sizzle reel = brand piece (direction and energy). Mac mini prototype = tangible demo (let people click through it). Neither is a shipping product today. Be honest about that. Honesty builds more trust than overselling.
Prospect Talk Track (Non-Clients)
Your go-to for someone who walks up and says “what do you guys do?”
“When Can I Get It?”
Qualifying for Early Access
We call them “design partners” internally – say “early access” externally.
What to look for
- Frustrated with their current EHR (especially ModMed)
- Willing to give feedback
- Comfortable being early
- Smaller practices (2–5 providers) that can move fast
Five Qualifying Questions
Strong candidate?
Get their info, note what they said, flag for Michael or Ashwin. “I’d love to connect you with our CEO Ashwin or our marketing lead Michael. They’re both here – can I set something up? And make sure you sign up at os.clarityrcm.com.”
ClarityOS Demo Script
4 screens, ~3 minutes. Ask their role first, then walk through.
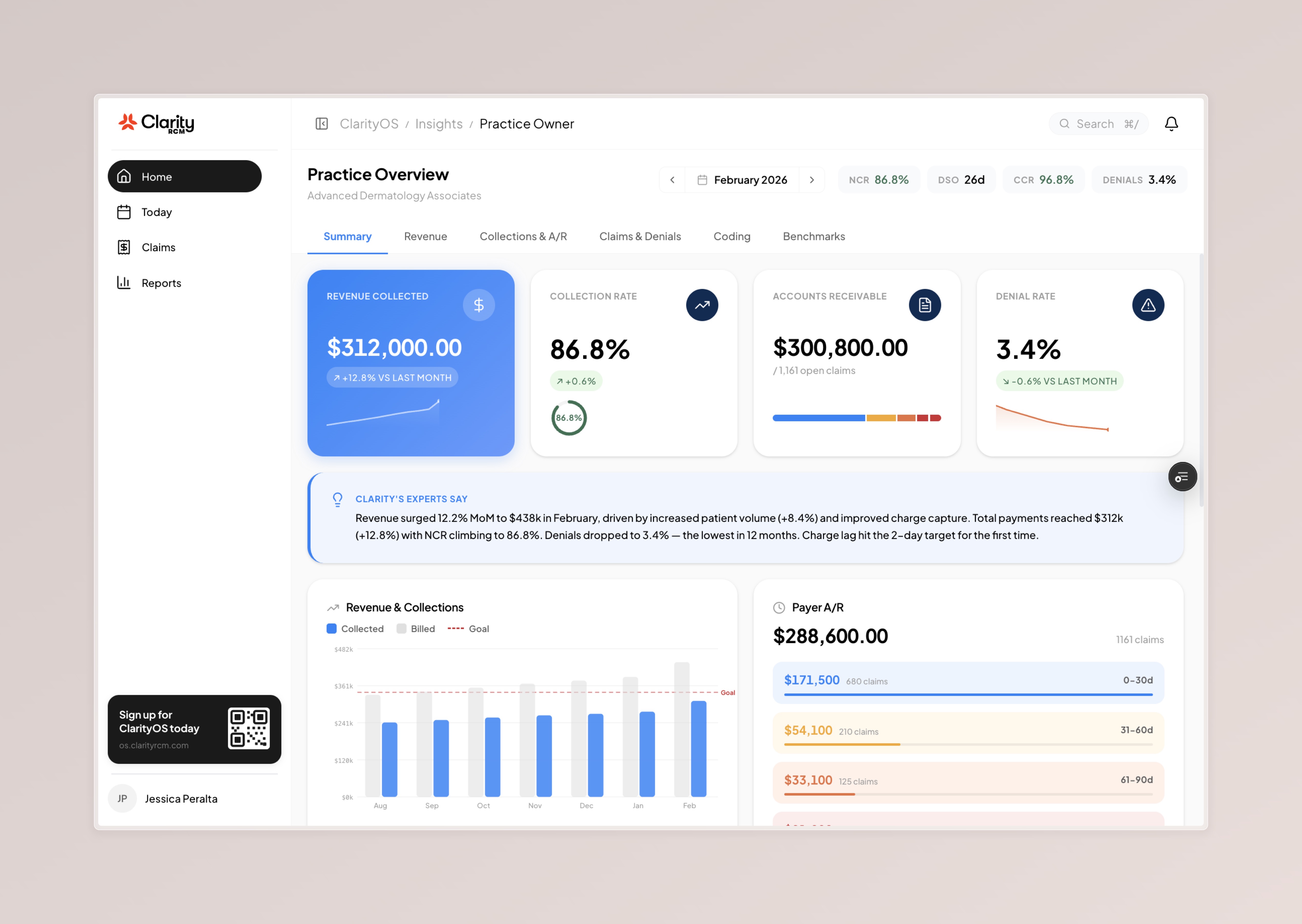
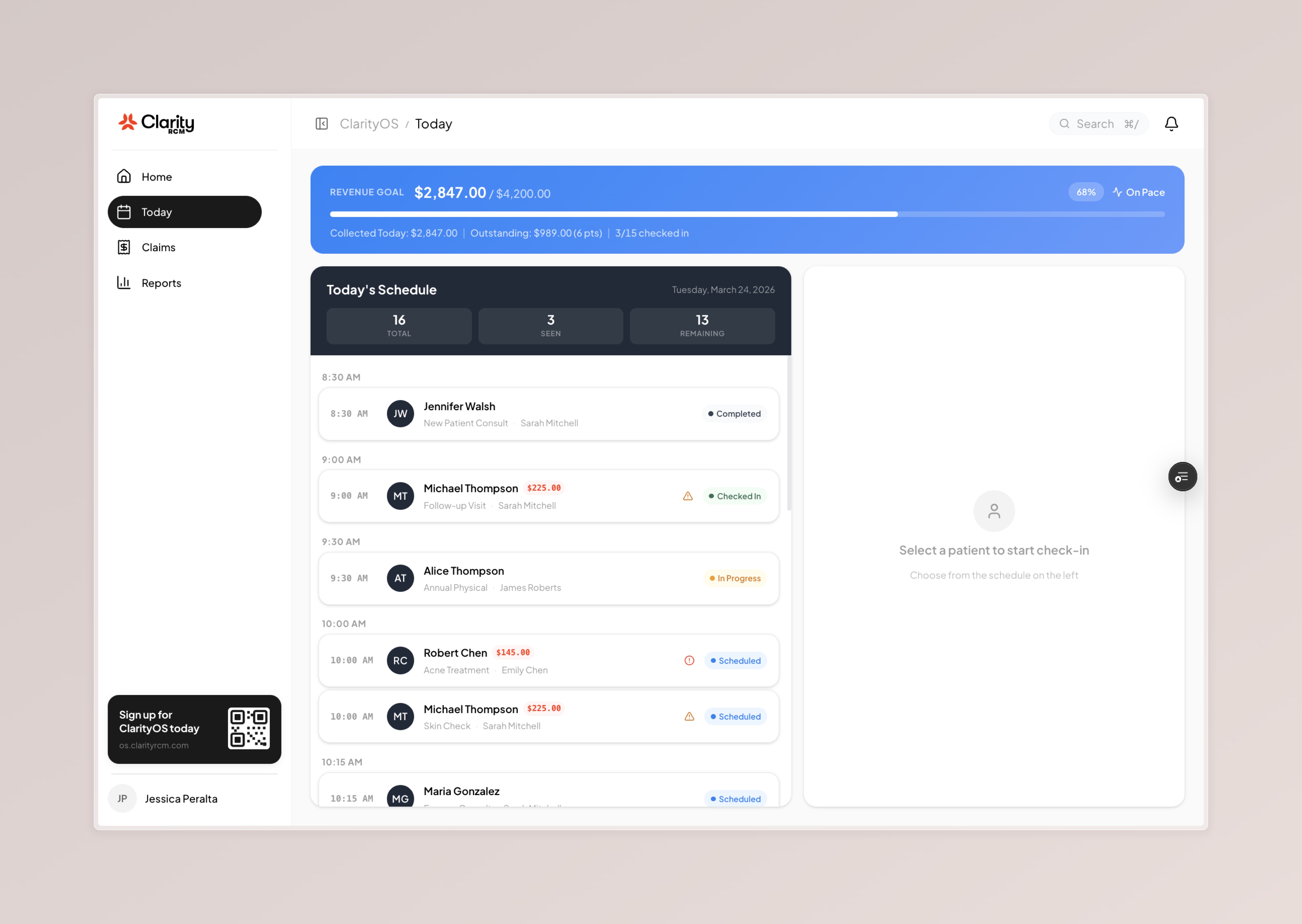
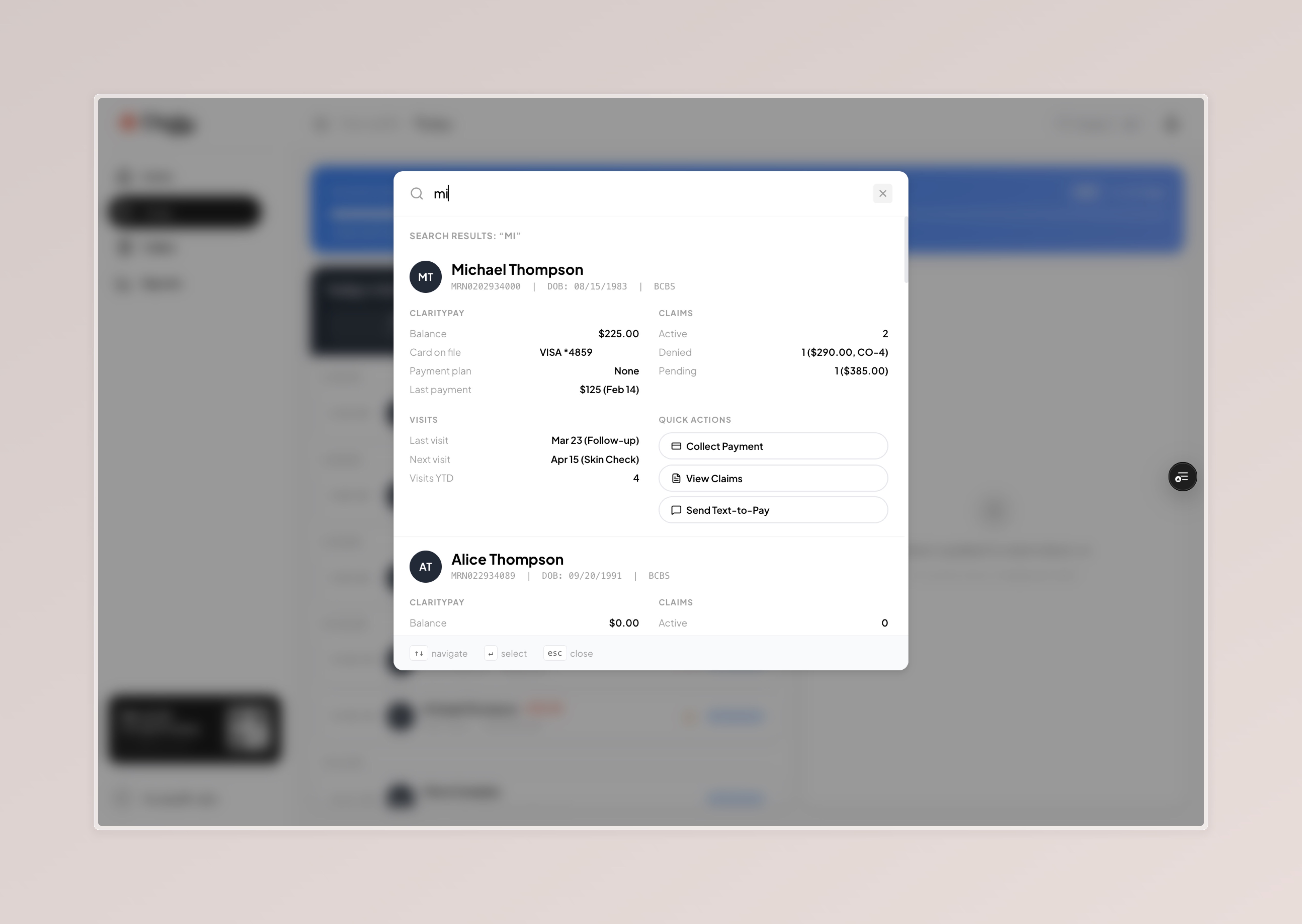
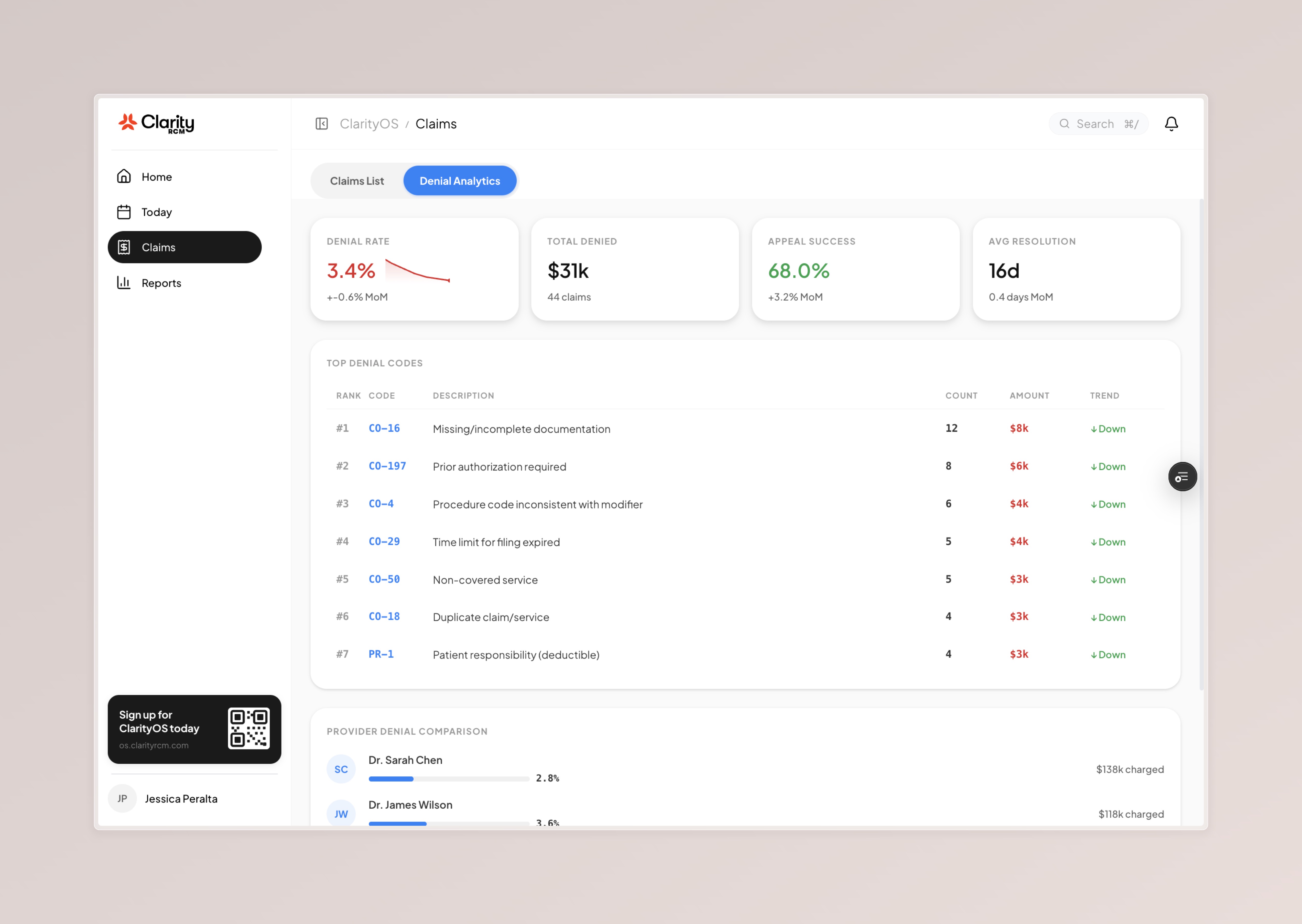
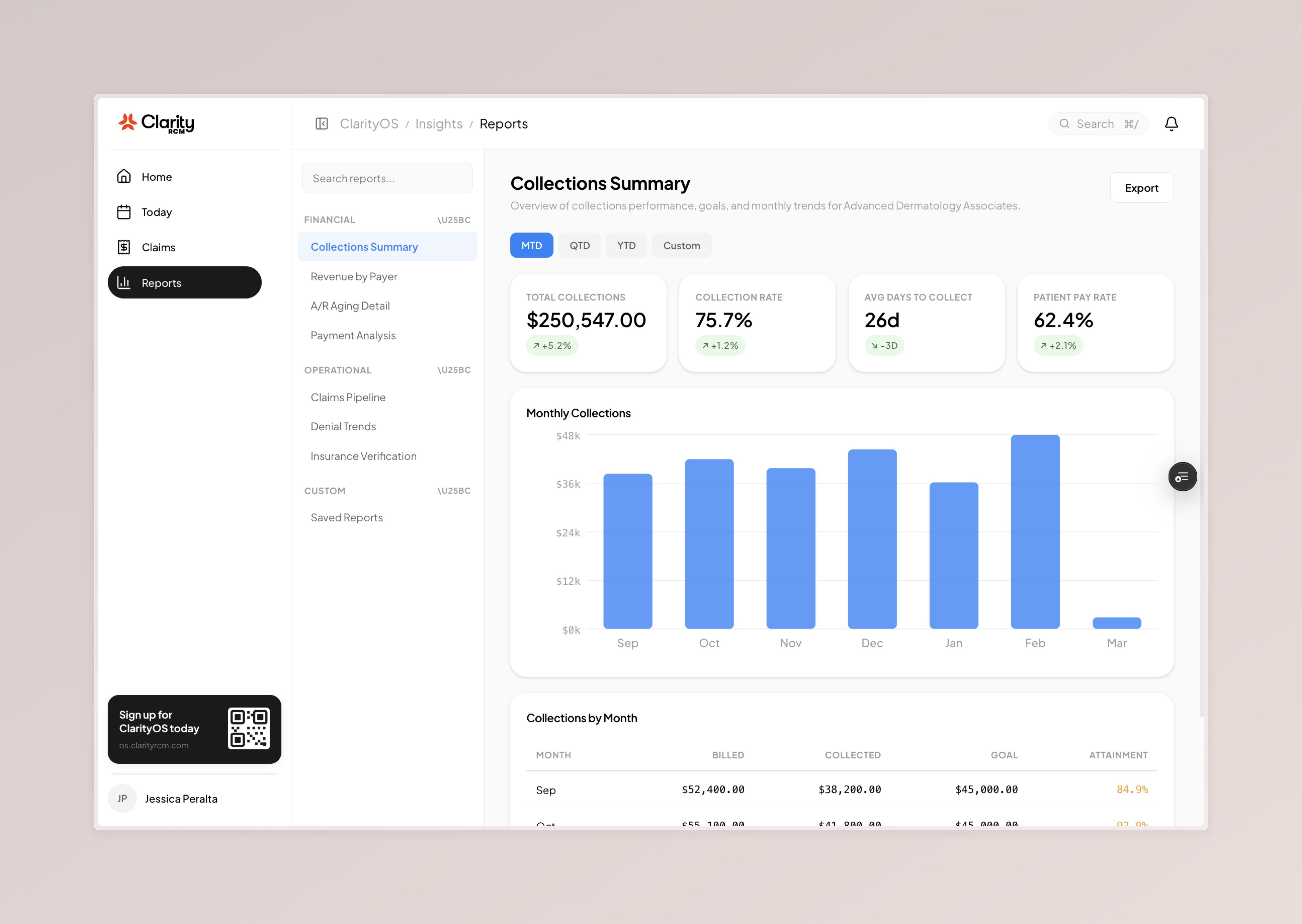
Close every demo with:
os.clarityrcm.comDemo Do’s and Don’ts
Do
- Ask what EHR they use before diving in
- Let them click around if they want to
- Be honest: “This is a prototype, not shipping yet”
- Connect features to their real problems
- End with os.clarityrcm.com sign-up
- Flag strong prospects to Michael or Ashwin
Don’t
- Promise specific features or dates
- Say “it will do X” unless it’s in the prototype
- Compare directly to ModMed or any EHR
- Spend more than 3 minutes unless they’re engaged
- Mention internal project names or infrastructure
- Let a strong prospect leave without getting their info
Post-AAD Launch Announcement
Who Reaches Out
| Segment | Who | Message | Ask |
|---|---|---|---|
| Happy clients | Their AM | “Exciting news, here’s what’s coming” | Early access interest |
| At-risk clients | AM + Lindsay | “We heard you, here’s what we’re building” | Reassurance + early access |
| Active prospects | AM or Michael | “You’re evaluating at the right time” | Demo + waitlist sign-up |
| Lapsed prospects | Michael | “Things have changed – worth another look” | Re-engagement + waitlist |
| Cold outreach | Michael / marketing | “Here’s what 200+ practices already know” | Website + waitlist |
Objection Handling
Scan this before a call. Find the objection, use the response.
What NOT to Say
Know where the lines are.
When to Escalate
| Situation | Who | How |
|---|---|---|
| Client wants detailed roadmap | Ashwin | Slack him with client name + what they asked |
| Strong early access candidate | Michael or Ashwin | Flag in #proj-clarity-os |
| Client mentions SubQ Docs | Use talk tracks above; escalate only if actively leaving | If leaving: flag in #sales-competitors + Lindsay + Ashwin immediately |
| Client asks about pricing specifics | Ashwin | Don’t speculate. Ashwin owns pricing |
| Client asks about EHR replacement | Michael or Ashwin | Slack either one |
| Large group prospect (6+ providers) | Ashwin in person | Grab him or text him |
| Media or analyst asks about ClarityOS | Michael immediately | Do NOT talk to press – text or Slack Michael |
| Client upset + mentions ClarityOS | Lindsay | Handle the real issue first. ClarityOS is a distraction |
| Someone asks about other specialties | Deflect – “We’re focused on dermatology” | If they push: Ashwin |
Quick Reference Card
“Next-generation RCM – autonomous where it needs to be, expert service where it matters. 200+ practices, 98% net collection rate. Sign up for early access at os.clarityrcm.com.”
“Same team, same results, now with real-time visibility. Things will look different a year from now.”
Calm, factual. They do the front of the visit. We do what happens after. Lots of companies do documentation well. Revenue cycle for independent derm is a different problem. Eight years of expertise.
“Meaningful progress within a year. Sign up at os.clarityrcm.com.”
“We’re building from the financial layer up. Lots of companies doing great clinical work. Our focus is getting independent derm practices paid.”
Ask Michael. That’s what he’s there for.
Every conversation – point them here:
os.clarityrcm.com